An official website of the United States government
 United States Department of Labor
United States Department of Labor
| December 2014
When Laura Hines began her career as a corrective therapist, the job title baffled people outside her workplace. “They’d ask, ‘Oh, you sell corrective shoes?’ or ‘You work in a correctional facility?’” she says. Her occupation later changed names, but that hasn’t clarified much. “Now we’re called kinesiotherapists,” says Laura, “and people are sometimes still confused.”
Kinesiology is the study of body-movement mechanics. Kinesiotherapists use rehabilitative exercise, reconditioning, and physical education to treat patients who have problems moving in any way. The career field emerged during World War II as a form of exercise therapy to treat service members’ injuries so that they could return to active duty.
Today, the physical reconditioning units where this therapy takes place are primarily in U.S. Department of Veterans Affairs (VA) facilities, where current and former military personnel may seek treatment.
Job duties for kinesiotherapists vary, depending on where they work—and sometimes within the facility itself. Responsibilities usually include assessing and treating patients, among other tasks.
Kinesiotherapists work under a physician’s direction, often with other specialists. For example, Laura is part of a team that also includes a nurse, a dietitian, and a social worker.
Assessment. To determine what exercises and training may be beneficial, a kinesiotherapist first evaluates patients to assess their physical abilities and activity levels. This assessment allows the kinesiotherapist to decide how much help, if any, patients need each day for routine tasks, such as walking, eating, and getting into and out of bed.
Home-care providers, like Laura, also do an environmental assessment of the patient’s residence to ensure safety. This includes evaluating a home’s potential safety risks—such as stairs, unsafe furniture, and nonworking smoke detectors—and recommending corrective action.
Treatment. Kinesiotherapists base a patient’s treatment plan on what they learned during assessment. Emphasizing the physical and psychological benefits of exercise, they focus on reconditioning and physical education. Treatment is tailored to each patient’s needs and situation.
For example, Laura had a patient with mobility problems who was limited to crawling in his own home. The patient could stand for only brief periods, so Laura created a plan that would help him rebuild strength gradually. “I started him on a treadmill for a few minutes at a time, because he needed to rest in between,” she says. Eventually, through reconditioning exercises with Laura’s guidance, the patient became fully mobile not just inside his house but out and about as well.
Other duties. In addition to tasks related to assessment and treatment, kinesiotherapists have some administrative duties. These include documenting patient visits; ordering equipment, such as adaptive-eating utensils or wheelchairs; and participating in outreach activities.
Some kinesiotherapists’ other responsibilities are related to the work but specific to their patient population. For example, Laura’s patients—whose average age is 83—often need help setting up electronic systems, such as a video monitor for patients with dementia who may wander away from home. “Some of my older patients are not tech savvy,” Laura says. “So if I order a monitor or some other system for them, I’ll go out and set it up.”
Kinesiotherapists need a bachelor’s or master’s degree, and the program must include a clinical internship. Professional registration is available to those who pass an exam. But kinesiotherapists also need some qualities that aren’t taught in school or tested on the exam.
Qualities. Kinesiotherapists need to be adaptable, enjoy people, and have patience and a good sense of humor. “You may have to work with patients who come from different eras and have different backgrounds,” Laura says. “You need to be comfortable working with all populations.”
Laura recommends that students considering kinesiotherapy contact the volunteer department of their local VA to find out if they can shadow a kinesiotherapist at work. Shadowing can help students get a feel for what kinesiotherapy is like and whether it suits them.
Education. Studying to become a kinesiotherapist involves a lot of sciences: anatomy, physiology, and physics, to name a few. Communications courses are also recommended for working with patients, documenting visits, and making outreach presentations.
There are only a handful of accredited kinesiotherapy programs at the bachelor’s degree level in the United States. Prospective kinesiotherapists may also get a master’s degree in exercise science or a related field. At either degree level, the program must include 1,000 hours of clinical internship in kinesiotherapy.
Registration. The American Kinesiotherapy Association offers professional registration for people who complete degree, instruction, and internship requirements and pass an exam. According to the association, most employers, including the VA, require that newly hired kinesiotherapists become registered and maintain registration through continuing education.
Working conditions vary for kinesiotherapists, depending on the type of work. According to the VA, most kinesiotherapists are employed by the Veterans Health Administration. Others work in establishments such as public and private hospitals or clinics, rehabilitation facilities, colleges and universities, and fitness or wellness centers.
Employment and wages. The Bureau of Labor Statistics does not collect employment or wage data on kinesiotherapists; instead, it counts them among exercise physiologists.
According to the American Kinesiotherapy Association, there currently are about 500 registered kinesiotherapists in the United States. The association has no way of counting how many unregistered kinesiotherapists there are. About 350 kinesiotherapists were employed by the Veterans Health Administration in 2011, according to the VA.
Because they work primarily in VA facilities, most kinesiotherapists are federal employees. The association estimates that these kinesiotherapists generally work at the GS-7 to GS-12 level, which had base pay of $34,319 and $60,877, respectively, in 2014.
Work environment. Kinesiotherapists’ work setting depends on the type of care they offer. Aquatic therapy takes place in pools, for example, and therapy for patients receiving psychiatric care is often provided in hospitals. Patient load and schedule also vary by location. Laura currently is responsible for about 90 to 100 patients.
In clinics, hospitals, and other settings, kinesiotherapists may have standard, 9-to-5 hours and work entirely onsite. Home-care kinesiotherapists travel to visit their patients instead of working in a fixed location.
For example, although Laura is based out of a VA facility in Tampa, Florida, she sets her own hours to visit patients in her territory. “I usually see patients from morning to early afternoon, then make my notes in the late afternoon,” she says. “I try to make my travel routes as efficient as possible so I’m not zigzagging all over.” Laura’s initial assessments take about 2 to 3 hours, but quarterly followup visits are shorter.
Kinesiotherapists’ paperwork can be time consuming, and the lack of occupational recognition outside of the VA is sometimes frustrating. But helping patients regain physical strength and mobility makes for a satisfying career. “It’s very rewarding when you work with someone and see that person’s situation improve,” says Laura. “I’ve been doing this for 28 years, and I’ve rarely woken up in the morning not wanting to go to work.”
Kathleen Green, "Kinesiotherapist," Career Outlook, U.S. Bureau of Labor Statistics, December 2014.
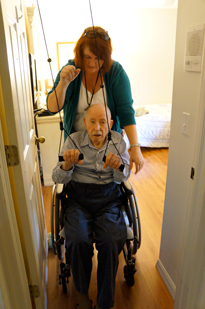
Kinesiotherapist Laura Hines uses rehabilitative exercises to work with a patient in his home. (Photo by Angela Black, RKT)