An official website of the United States government
 United States Department of Labor
United States Department of Labor

Crossref 0
The Road Home: Predictors of Health Care Utilization Among Older Returning African American Men, The Review of Black Political Economy, 2021.
Developing a Set of Uniform Outcome Measures for Adult Day Services, Journal of Applied Gerontology, 2020.
In 2015, employment in the health care and social assistance sector grew by 3.5 percent, outpacing total nonfarm job growth. A large part of this employment gain was driven by community-based care industries, which include home health care services, services for the elderly and persons with disabilities, and community care facilities for the elderly. These industries are adding jobs at a rapid pace as the older population in the United States grows and seeks out affordable care options.
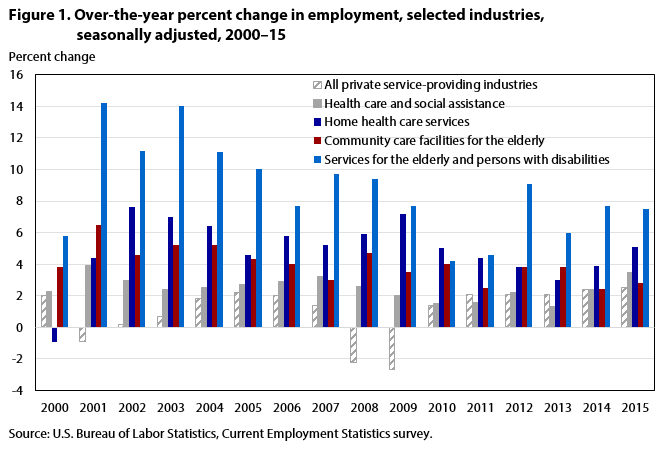
| Year | All private service-providing industries | Health care and social assistance | Home health care services | Community care facilities for the elderly | Services for the elderly and persons with disabilities |
|---|---|---|---|---|---|
| 2000 | 2.0 | 2.3 | -0.9 | 3.8 | 5.8 |
| 2001 | -.9 | 3.9 | 4.4 | 6.5 | 14.2 |
| 2002 | .2 | 3.0 | 7.6 | 4.6 | 11.2 |
| 2003 | .7 | 2.4 | 7.0 | 5.2 | 14.0 |
| 2004 | 1.8 | 2.5 | 6.4 | 5.2 | 11.1 |
| 2005 | 2.2 | 2.7 | 4.6 | 4.3 | 10.0 |
| 2006 | 2.0 | 2.9 | 5.8 | 4.0 | 7.7 |
| 2007 | 1.4 | 3.2 | 5.2 | 3.0 | 9.7 |
| 2008 | -2.2 | 2.6 | 5.9 | 4.7 | 9.4 |
| 2009 | -2.7 | 2.0 | 7.2 | 3.5 | 7.7 |
| 2010 | 1.4 | 1.5 | 5.0 | 4.0 | 4.2 |
| 2011 | 2.1 | 1.6 | 4.4 | 2.5 | 4.6 |
| 2012 | 2.1 | 2.2 | 3.8 | 3.8 | 9.1 |
| 2013 | 2.1 | 1.3 | 3.0 | 3.8 | 6.0 |
| 2014 | 2.4 | 2.4 | 3.9 | 2.4 | 7.7 |
| 2015 | 2.5 | 3.5 | 5.1 | 2.8 | 7.5 |
| Source: U.S. Bureau of Labor Statistics, Current Employment Statistics survey. | |||||
In 2015, health care and social assistance, an industry sector known for its economic robustness even during times of recession,1 added jobs at its fastest rate since 2001, outpacing employment growth in all private service-providing industries.2 (See figure 1.) Over the year, some of the sector’s most rapid employment growth occurred in industries that provide elder care outside of nursing homes. Two of those industries—services for the elderly and persons with disabilities, and home health care services—far outpaced employment growth in health care and social assistance. Employment in a third industry—community care facilities for the elderly—outpaced employment growth for all private service-providing industries combined.
Given recent increases in the U.S. population ages 65 and older, the job growth seen in industries that provide health care and social assistance to the elderly is not surprising. Steady demand for long-term care services translates into a greater need for health care and social assistance workers. This article details these employment trends and the demographic, economic, and legislative changes associated with them.
According to the U.S. Department of Health and Human Services, home and community services provide elderly individuals, as well as physically or mentally disabled people of all ages, with assistance in their daily activities, both at home and in community-based settings.3 These services are delivered primarily by providers in three industries classified in accordance with the North American Industry Classification System (NAICS):
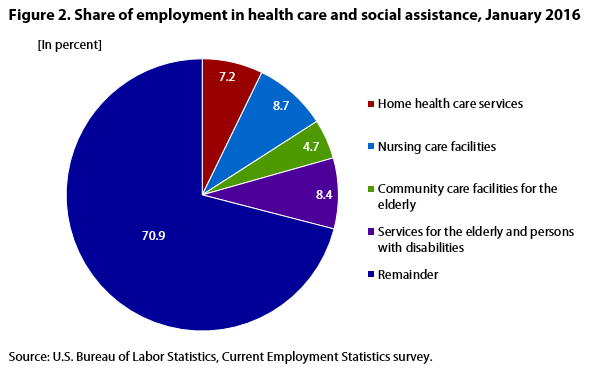
| Industry | Share of employment |
|---|---|
| Home health care services | 7.2 |
| Nursing care facilities | 8.7 |
| Community care facilities for the elderly | 4.7 |
| Services for the elderly and persons with disabilities | 8.4 |
| Remainder | 70.9 |
| Source: U.S. Bureau of Labor Statistics, Current Employment Statistics survey. | |
These three industries (hereafter referred to collectively as “community-based care industries”), along with nursing care facilities, make up the industries that provide long-term care services (primarily to the elderly) in the health care and social assistance sector. Combined, these long-term care industries account for nearly 30 percent of the sector’s employment. (See figure 2.)
Community-based care industries have seen some of the strongest employment growth in recent years. In 2015, employment in services for the elderly and persons with disabilities and in home health care services increased by 7.5 percent and 5.0 percent, respectively, outpacing job growth in health care and social assistance (3.5 percent). Employment in community care facilities for the elderly increased by 2.9 percent in 2015. These recent job gains reflect long-term trends of employment expansion in community-based care industries, which have been steadily adding jobs since 1990.
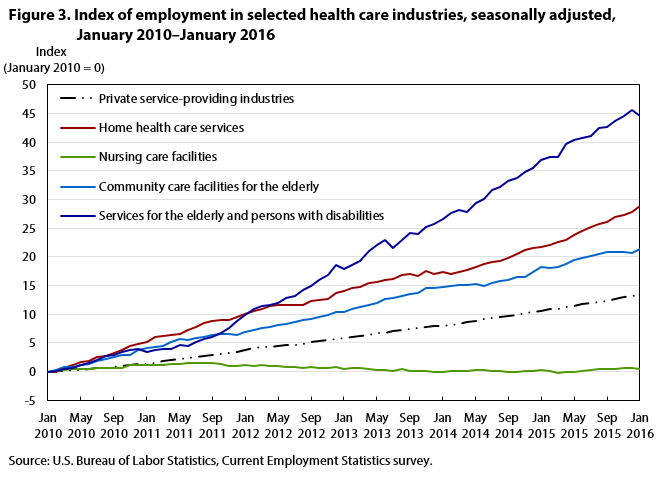
| Date | Private service-providing industries | Home health care services | Nursing care facilities | Community care facilities for the elderly | Services for the elderly and persons with disabilities |
|---|---|---|---|---|---|
| Jan 2010 | 0.00 | 0.00 | 0.00 | 0.00 | 0.00 |
| Feb 2010 | .03 | -.12 | .15 | .27 | .15 |
| Mar 2010 | .11 | .68 | .32 | .75 | .45 |
| Apr 2010 | .26 | 1.20 | .43 | .84 | .72 |
| May 2010 | .36 | 1.61 | .44 | 1.08 | 1.12 |
| Jun 2010 | .47 | 1.84 | .41 | 1.36 | 1.44 |
| Jul 2010 | .57 | 2.54 | .62 | 1.78 | 2.11 |
| Aug 2010 | .68 | 2.74 | .66 | 2.15 | 2.76 |
| Sep 2010 | .82 | 3.24 | .66 | 2.51 | 2.96 |
| Oct 2010 | 1.03 | 3.85 | .71 | 2.84 | 3.45 |
| Nov 2010 | 1.15 | 4.45 | 1.14 | 2.89 | 3.72 |
| Dec 2010 | 1.31 | 4.82 | 1.21 | 3.76 | 3.96 |
| Jan 2011 | 1.38 | 5.13 | 1.24 | 4.15 | 3.44 |
| Feb 2011 | 1.57 | 5.99 | 1.18 | 4.22 | 3.73 |
| Mar 2011 | 1.78 | 6.23 | 1.23 | 4.52 | 3.98 |
| Apr 2011 | 2.12 | 6.46 | 1.26 | 5.17 | 3.97 |
| May 2011 | 2.20 | 6.48 | 1.28 | 5.74 | 4.66 |
| Jun 2011 | 2.38 | 7.28 | 1.50 | 5.51 | 4.44 |
| Jul 2011 | 2.54 | 7.84 | 1.44 | 5.85 | 5.09 |
| Aug 2011 | 2.66 | 8.44 | 1.49 | 6.02 | 5.69 |
| Sep 2011 | 2.92 | 8.88 | 1.53 | 6.39 | 5.98 |
| Oct 2011 | 3.11 | 9.04 | 1.40 | 6.59 | 6.75 |
| Nov 2011 | 3.30 | 8.96 | .98 | 6.59 | 7.57 |
| Dec 2011 | 3.49 | 9.46 | .96 | 6.33 | 8.79 |
| Jan 2012 | 3.81 | 10.04 | 1.11 | 6.84 | 9.94 |
| Feb 2012 | 4.07 | 10.53 | .92 | 7.29 | 10.84 |
| Mar 2012 | 4.28 | 10.97 | 1.21 | 7.57 | 11.44 |
| Apr 2012 | 4.37 | 11.37 | .96 | 7.75 | 11.63 |
| May 2012 | 4.51 | 11.57 | 1.00 | 8.06 | 11.97 |
| Jun 2012 | 4.56 | 11.65 | .86 | 8.32 | 12.76 |
| Jul 2012 | 4.70 | 11.69 | .89 | 8.65 | 13.23 |
| Aug 2012 | 4.89 | 11.63 | .56 | 8.99 | 14.29 |
| Sep 2012 | 5.10 | 12.32 | .73 | 9.20 | 14.92 |
| Oct 2012 | 5.26 | 12.58 | .59 | 9.56 | 16.05 |
| Nov 2012 | 5.45 | 12.64 | .56 | 9.86 | 16.84 |
| Dec 2012 | 5.64 | 13.66 | .79 | 10.41 | 18.67 |
| Jan 2013 | 5.82 | 14.07 | .42 | 10.47 | 17.97 |
| Feb 2013 | 6.07 | 14.58 | .61 | 10.95 | 18.54 |
| Mar 2013 | 6.21 | 14.79 | .55 | 11.24 | 19.37 |
| Apr 2013 | 6.43 | 15.40 | .50 | 11.54 | 21.02 |
| May 2013 | 6.65 | 15.72 | .35 | 12.01 | 22.01 |
| Jun 2013 | 6.82 | 15.90 | .30 | 12.65 | 22.95 |
| Jul 2013 | 7.02 | 16.19 | .07 | 12.89 | 21.50 |
| Aug 2013 | 7.23 | 16.89 | .53 | 13.20 | 22.98 |
| Sep 2013 | 7.38 | 16.96 | .05 | 13.60 | 24.20 |
| Oct 2013 | 7.56 | 16.68 | .17 | 13.76 | 23.96 |
| Nov 2013 | 7.81 | 17.51 | .07 | 14.57 | 25.29 |
| Dec 2013 | 7.89 | 17.05 | -.01 | 14.66 | 25.78 |
| Jan 2014 | 8.03 | 17.34 | -.02 | 14.71 | 26.69 |
| Feb 2014 | 8.16 | 17.00 | .12 | 15.00 | 27.72 |
| Mar 2014 | 8.39 | 17.44 | .04 | 15.11 | 28.17 |
| Apr 2014 | 8.63 | 17.64 | .18 | 15.19 | 27.77 |
| May 2014 | 8.85 | 18.32 | .22 | 15.36 | 29.38 |
| Jun 2014 | 9.10 | 18.74 | .29 | 14.88 | 30.17 |
| Jul 2014 | 9.30 | 19.03 | .18 | 15.40 | 31.62 |
| Aug 2014 | 9.51 | 19.26 | .08 | 15.77 | 32.23 |
| Sep 2014 | 9.73 | 19.86 | .02 | 15.94 | 33.26 |
| Oct 2014 | 9.90 | 20.49 | .00 | 16.58 | 33.69 |
| Nov 2014 | 10.20 | 21.14 | .04 | 16.59 | 34.74 |
| Dec 2014 | 10.44 | 21.59 | .05 | 17.45 | 35.49 |
| Jan 2015 | 10.62 | 21.76 | .27 | 18.18 | 36.90 |
| Feb 2015 | 10.88 | 22.15 | .15 | 18.04 | 37.51 |
| Mar 2015 | 11.00 | 22.68 | -.23 | 18.25 | 37.48 |
| Apr 2015 | 11.25 | 22.88 | -.03 | 18.77 | 39.72 |
| May 2015 | 11.53 | 23.81 | -.02 | 19.39 | 40.39 |
| Jun 2015 | 11.78 | 24.59 | .03 | 19.80 | 40.75 |
| Jul 2015 | 12.04 | 25.18 | .27 | 20.19 | 41.15 |
| Aug 2015 | 12.20 | 25.79 | .41 | 20.47 | 42.49 |
| Sep 2015 | 12.40 | 26.09 | .53 | 20.89 | 42.71 |
| Oct 2015 | 12.70 | 26.97 | .53 | 20.91 | 43.76 |
| Nov 2015 | 12.96 | 27.24 | .66 | 20.92 | 44.56 |
| Dec 2015 | 13.20 | 27.79 | .69 | 20.77 | 45.62 |
| Jan 2016 | 13.34 | 28.81 | .42 | 21.31 | 44.61 |
| Source: U.S. Bureau of Labor Statistics, Current Employment Statistics survey. | |||||
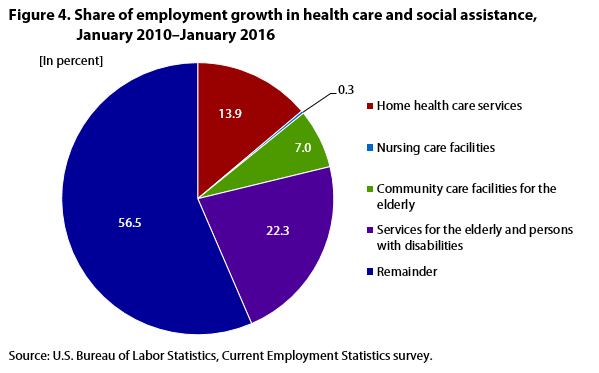
| Industry | Share of employment growth |
|---|---|
| Home health care services | 13.9 |
| Nursing care facilities | .3 |
| Community care facilities for the elderly | 7.0 |
| Services for the elderly and persons with disabilities | 22.3 |
| Remainder | 56.5 |
| Source: U.S. Bureau of Labor Statistics, Current Employment Statistics survey. | |
As shown in figure 3, employment in services for the elderly and persons with disabilities had the largest increase among the community-based care industries, rising from 1.1 million in January 2010 to 1.6 million in January 2016, an increase of 45 percent.5 Over the same period, employment in home health care services and in community care facilities for the elderly also recorded strong growth, increasing from 1.1 million to 1.4 million (29 percent) and from 729,000 to 885,000 (22 percent), respectively. Combined, community-based care industries accounted for nearly half of the job gain in health care and social assistance during the period. (See figure 4.)
| Industry | Average weekly earnings | Employment (thousands) | Percent change in employment (January 2010–January 2016) |
|---|---|---|---|
| Offices of physicians | $1,354.82 | 2,588.0 | 12.18 |
| Dentists | 860.42 | 929.4 | 13.42 |
| Other health practitioners | 737.76 | 842.2 | 28.38 |
| Outpatient care centers | 976.28 | 767.1 | 31.38 |
| Medical and diagnostic labs | 1,089.65 | 259.1 | 15.77 |
| Home health care services | 547.61 | 1,379.8 | 30.08 |
| Other ambulatory health care | 832.15 | 293.5 | 18.25 |
| General medical hospitals | 1,153.31 | 4,629.8 | 5.99 |
| Psychiatric hospitals | 822.08 | 143.3 | 34.93 |
| Other hospitals | 985.30 | 269.6 | 33.80 |
| Nursing care facilities | 593.48 | 1,652.0 | .22 |
| Residential mental health facilities | 550.14 | 613.9 | 9.20 |
| Community care facilities for the elderly | 515.82 | 889.4 | 21.94 |
| Other residential care facilities | 604.44 | 163.3 | 1.62 |
| Services for the elderly and persons with disabilities | 402.64 | 1,601.7 | 45.23 |
| Private service-providing industries | 838.49 | 101,985.0 | 13.82 |
| Source: U.S. Bureau of Labor Statistics, Current Employment Statistics survey. | |||
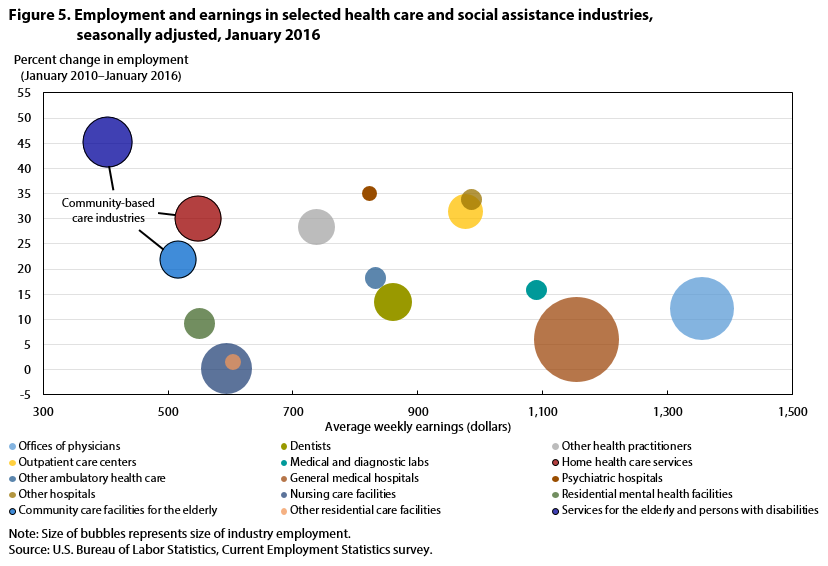
Although community-based care industries are topping others in job growth, their workers have some of the lowest earnings.6 Average weekly earnings in community-based care industries are well below those in total private service-providing industries and in most other health care industries. (See figure 5.) Because community-based care industries do not focus primarily on providing medical services, the occupations that make up their employment are mostly nonmedical and typically do not require any formal education credential. Lower educational attainment is, in turn, correlated with lower wages.
According to data from the Occupational Employment Statistics survey, a few similar, low-wage occupations make up the greatest share of jobs in community-based care industries. Two of the most common occupations in each community-based care industry are personal care aides, who “assist the elderly, convalescents, or persons with disabilities with daily living activities at the person's home or in a care facility,” and home health aides, who “provide routine individualized healthcare…to the elderly, convalescents, or persons with disabilities at the patient's home or in a care facility….”7 These occupations do not typically require an educational credential for entry, and the workers employed in them receive median annual wages between $19,000 and $23,000, depending on the industry.8 (See table 1.)
| Occupational title | Total employment | Percent of total employment | Median hourly wage | Annual median wage | Typical education needed for entry |
|---|---|---|---|---|---|
| Home health care services | |||||
| Home health aides | 385,440 | 29.67 | $10.44 | $21,710 | No formal educational credential |
| Personal care aides | 298,450 | 22.98 | 9.2 | 19,130 | No formal educational credential |
| Registered nurses | 173,590 | 13.36 | 30.69 | 63,840 | Bachelor's degree |
| Community care facilities for the elderly | |||||
| Nursing assistants | 156,220 | 18.11 | 11.64 | 24,200 | Postsecondary nondegree award |
| Personal care aides | 127,470 | 14.77 | 10.3 | 21,410 | No formal educational credential |
| Home health aides | 95,590 | 11.08 | 10.67 | 22,200 | No formal educational credential |
| Services for the elderly and persons with disabilities | |||||
| Personal care aides | 543,510 | 53.98 | 10.13 | 21,070 | No formal educational credential |
| Home health aides | 142,910 | 14.19 | 10.34 | 21,500 | No formal educational credential |
| Social and human service assistants | 29,360 | 2.92 | 14.92 | 31,030 | High school diploma |
| Source: U.S. Bureau of Labor Statistics, Occupational Employment Statistics survey and Employment Projections program. | |||||
In addition to having a high concentration of low-wage occupations, community-based care industries have a high concentration of female workers. In community care facilities for the elderly, home health care services, and services for the elderly and persons with disabilities, women make up 81 percent, 88 percent, and 84 percent, respectively, of total employment. By comparison, women make up 53 percent of total employment in private service-providing industries.
The most common community-based care occupations are projected to be among the fastest growing over the 2014–24 decade. Within that period, personal care aides is expected to add the greatest number of jobs (458,100) of any occupation.9 Home health aides is expected to be the fifth-fastest-growing occupation, with a 38.1-percent increase in employment, and to add the third-greatest number of jobs (348,400). Nursing assistants and registered nurses—among the most common occupations in community care facilities for the elderly and in home health care services—are expected to add 262,000 and 439,300 jobs, respectively.
The strong job growth in community-based care industries reflects an increased demand for their services—a demand that coincides with recent demographic and economic trends in the United States. One of these trends is the rise in the population of people over age 65. Another is the growing appeal of receiving care in community-based settings, which, unlike nursing care facilities (commonly known as nursing homes), allow people to remain in the comfort of their communities while receiving services.
In addition, lower costs for care providers in community-based care industries lead to lower costs for care recipients and, in turn, to increased demand for community-based care services. Although facilities such as nursing homes offer alternative options for long-term care, these options tend to be more expensive, because inpatient facilities have to provide room and board and require costly medical equipment and staff that can serve people with greater medical and self-care needs. Lastly, recent legislative changes pertaining to Medicare and Medicaid services—changes introduced as part of the Affordable Care Act
| Year | Population level | |
|---|---|---|
| 65 to 84 years | 85 years and older | |
| 1990 | 28,061,429 | 3,022,021 |
| 1991 | 28,622,485 | 3,189,139 |
| 1992 | 29,041,334 | 3,314,660 |
| 1993 | 29,456,245 | 3,445,566 |
| 1994 | 29,769,771 | 3,561,032 |
| 1995 | 30,088,582 | 3,680,722 |
| 1996 | 30,348,157 | 3,794,892 |
| 1997 | 30,496,085 | 3,905,476 |
| 1998 | 30,586,624 | 4,032,535 |
| 1999 | 30,643,823 | 4,154,018 |
| 2000 | 30,807,096 | 4,262,472 |
| 2001 | 30,977,797 | 4,312,494 |
| 2002 | 31,153,399 | 4,368,808 |
| 2003 | 31,397,353 | 4,466,176 |
| 2004 | 31,657,436 | 4,545,883 |
| 2005 | 31,956,499 | 4,693,299 |
| 2006 | 32,298,178 | 4,865,929 |
| 2007 | 32,786,166 | 5,039,545 |
| 2008 | 33,581,781 | 5,195,840 |
| 2009 | 34,255,874 | 5,367,301 |
| 2010 | 34,936,483 | 5,542,810 |
| 2011 | 35,664,438 | 5,701,527 |
| 2012 | 37,283,786 | 5,877,486 |
| 2013 | 38,665,848 | 6,013,334 |
| 2014 | 40,060,959 | 6,140,771 |
| 2015 | 41,473,691 | 6,287,161 |
| Source: U.S. Census Bureau. | ||
| Year | Population change (percent) | |
|---|---|---|
| 65 to 84 years | 85 years and older | |
| 1990 | 2.0 | 5.5 |
| 1991 | 1.5 | 3.9 |
| 1992 | 1.4 | 3.9 |
| 1993 | 1.1 | 3.4 |
| 1994 | 1.1 | 3.4 |
| 1995 | 0.9 | 3.1 |
| 1996 | 0.5 | 2.9 |
| 1997 | 0.3 | 3.3 |
| 1998 | 0.2 | 3.0 |
| 1999 | 0.5 | 2.6 |
| 2000 | 0.6 | 1.2 |
| 2001 | 0.6 | 1.3 |
| 2002 | 0.8 | 2.2 |
| 2003 | 0.8 | 1.8 |
| 2004 | 0.9 | 3.2 |
| 2005 | 1.1 | 3.7 |
| 2006 | 1.5 | 3.6 |
| 2007 | 2.4 | 3.1 |
| 2008 | 2.0 | 3.3 |
| 2009 | 2.0 | 3.3 |
| 2010 | 2.1 | 2.9 |
| 2011 | 4.5 | 3.1 |
| 2012 | 3.7 | 2.3 |
| 2013 | 3.6 | 2.1 |
| 2014 | 3.5 | 2.4 |
| Source: U.S. Census Bureau. | ||
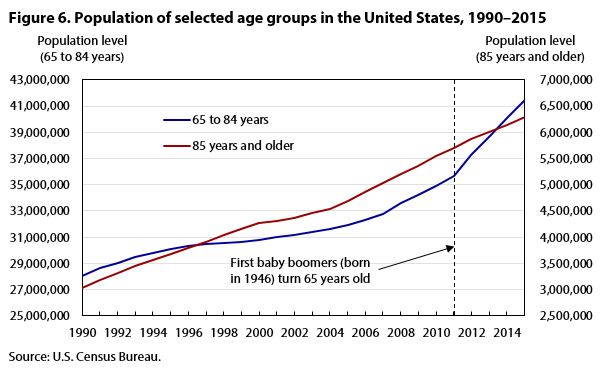
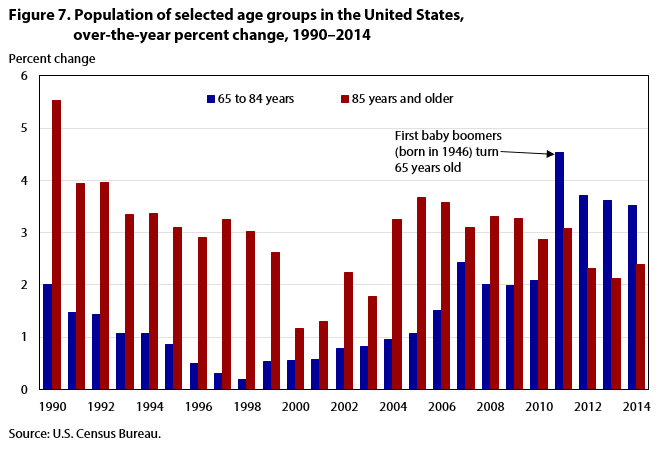
The employment increases in community-based care industries coincide with growth in the population of older Americans served by those industries. The number of noninstitutionalized adults 65 years and older in the United States now stands at 47.8 million, compared with 8.8 million in 2003.10 (See figures 6 and 7.) By 2040, their number is expected to reach 82.3 million.11 This expansion can be attributed mostly to the aging of the baby-boom generation (those born between 1946 and 1964), which represents one of the largest age demographics in the United States. The oldest people in this demographic are now 71 years old, and individuals in older age groups typically require more care for health-related issues. Among noninstitutionalized Americans ages 65 and over, more than one-third have some type of disability and 15 percent report having independent-living difficulty. In addition, about one-third of older Americans live alone and may not have anyone to assist them if they do have or do develop a disability.12 There are currently millions of aging U.S. adults with some type of need that could be met with services provided by community-based care providers, and that number will continue to grow.
The need for medical care and social assistance for older people in the United States is further reflected in spending data for the group. According to data from the Consumer Expenditure Survey, individuals ages 65 and older spent an average of $954 on medical services in 2014, compared with $790 for the total U.S. population.13 This difference demonstrates that an increased need for medical services translates into increased expenditures, some of which are for services provided by community-based care industries.
Basic economics suggests that, if presented with two similar but differently priced goods or services, consumers will be more likely to purchase the cheaper good or service. Data from private surveys demonstrate that, on average, community-based care is currently less expensive to consumers than traditional residential long-term care. According to the Cost of Care Survey conducted by Genworth Financial, Inc., an insurance company that provides long-term care products, the cost of adult daycare in the United States averaged $17,904 in 2015.14 For homemaker services, home health aide services, and assisted living facilities—all in the middle of the price range for long-term care—that cost averaged around $45,000. Nursing home care was at the top of the price range, with an average annual cost of $80,300 for a semiprivate room and $91,250 for a private room. Although community-based care services are not always a perfect substitute for inpatient services provided by hospitals and nursing homes, their lower cost is enough to motivate consumers to choose them whenever possible.
Expectations of future prices also affect demand for goods and services. Over the last 10 years, prices for consumers have increased at a much slower rate in community-based care than in other long-term care services. According to Consumer Price Index data, the price for care of invalids and elderly at home, a service that is provided primarily by community-based care industries, increased moderately, by 19.3 percent from December 2005 to December 2015.15 In contrast, over the same period, the price of inpatient hospital services rose by 69.8 percent and the price of nursing home and adult daycare services rose by 41.7 percent. Thus, the cost of community-based care services has increased at a slower pace than the cost of services provided by inpatient health care industries, such as hospitals and nursing homes. This price stability allows consumers to better plan their finances around community-based services and, thus, increases the attractiveness of those services.
| Year | Enrollees (millions) |
|---|---|
| 1990 | 22.8 |
| 1991 | 25.9 |
| 1992 | 28.5 |
| 1993 | 30.5 |
| 1994 | 31.7 |
| 1995 | 32.3 |
| 1996 | 32.2 |
| 1997 | 31.8 |
| 1998 | 31.4 |
| 1999 | 32.2 |
| 2000 | 34.2 |
| 2001 | 36.8 |
| 2002 | 40.4 |
| 2003 | 43.0 |
| 2004 | 44.5 |
| 2005 | 45.8 |
| 2006 | 45.6 |
| 2007 | 45.6 |
| 2008 | 47.2 |
| 2009 | 50.8 |
| 2010 | 54.3 |
| 2011 | 55.9 |
| 2012 | 57.2 |
| 2013 | 58.2 |
| 2014 | 65.9 |
| Source: U.S. Department of Health and Human Services. | |
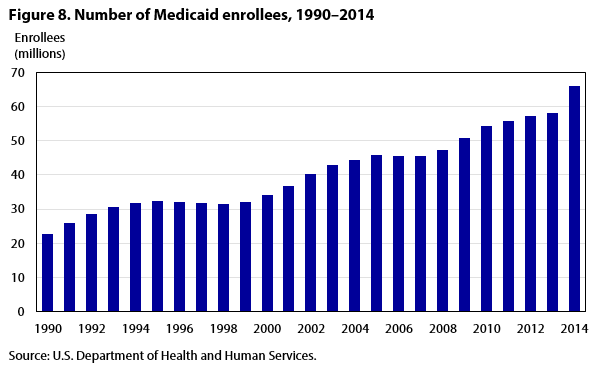
Historically, Medicaid and Medicare legislative changes aimed at increasing funding for community-based care industries have coincided with employment increases in those industries, especially home health care. In 1988, the ruling in the Duggan v. Bowen lawsuit,16 which challenged the administration of the Medicare home health care program, substantially increased Medicare funding for home health care services. Spending for the industry’s services rose rapidly from 1990 to 1997, as did its employment.17 Recent ACA-related changes to Medicaid laws reflect a further transition of government financial support toward community-based care, driving its job growth. These legislative changes occurred in tandem with increases in both Medicaid enrollment (see figure 8) and the U.S. population ages 65 and older.
Several major rulings since the implementation of the ACA have created programs to increase the funding for, and the accessibility of, community-based care services in eligible states that chose to participate in those programs. On October 1, 2010, the implementation of ACA amendment 1915(i), State Plan Home and Community-Based Services, provided states with new options for offering community-based care services through Medicaid state plans and increased the income ceiling for households that may receive the services.18 According to a letter from the U.S. Department of Health and Human Services to state Medicaid directors, the purpose of the change was to add “a new section to 1915(i) that allows States the option of providing services to individuals with income up to 300 percent of the Supplemental Security Income (SSI) Federal benefit rate (FBR).”19 The final ruling for this amendment took place on January 16, 2014.20
In addition, new Medicaid provisions implemented as part of ACA amendment 1915(k), Community First Choice Option, likely had an impact on the accessibility of community-based care services. These provisions increased federal–state Medicaid matching payments for community-based care services for people at risk of institutional care as a way to incentivize states to make those services more accessible. The final ruling for this amendment took place on July 6, 2012, stating the following about the amendment’s purpose and provisions:
The Community First Choice Option established a new State plan option to provide home and community-based attendant services and supports at a 6 percentage point increase in Federal medical assistance percentage (FMAP)…. States electing this option must make available home and community-based attendant services and supports to assist in accomplishing activities of daily living…and health-related tasks through hands-on assistance, supervision, and/or cueing.21
| Date | Texas | Pennsylvania | New York | Massachusetts | New Jersey | California | Florida | Louisiana | Michigan |
|---|---|---|---|---|---|---|---|---|---|
| Jan 2010 | 0.00 | 0.00 | 0.00 | 0.00 | 0.00 | 0.00 | 0.00 | 0.00 | 0.00 |
| Feb 2010 | .51 | -1.13 | .18 | .00 | -.88 | 1.32 | .95 | .98 | .60 |
| Mar 2010 | 1.75 | .56 | 1.47 | .73 | .29 | 2.32 | 1.27 | 2.44 | 1.50 |
| Apr 2010 | 2.80 | 1.41 | 3.03 | 1.09 | 1.76 | 2.98 | 2.38 | 3.90 | 1.80 |
| May 2010 | 3.63 | 3.94 | 3.67 | 2.19 | 2.94 | 3.64 | 3.17 | 4.88 | 3.29 |
| Jun 2010 | 4.13 | 2.25 | 5.32 | 2.92 | 2.94 | 3.48 | 2.70 | 5.37 | 2.10 |
| Jul 2010 | 3.90 | 3.38 | 4.40 | 4.01 | 3.53 | 3.31 | 2.54 | 8.78 | 2.99 |
| Aug 2010 | 4.59 | 4.23 | 5.32 | 4.38 | 4.12 | 3.64 | 2.38 | 8.78 | 4.19 |
| Sep 2010 | 5.24 | 5.35 | 6.33 | 4.01 | 6.18 | 3.64 | 1.90 | 8.29 | 3.59 |
| Oct 2010 | 5.56 | 5.63 | 8.81 | 6.57 | 7.35 | 4.97 | 3.97 | 9.27 | 6.29 |
| Nov 2010 | 6.06 | 6.76 | 10.18 | 6.93 | 9.41 | 5.46 | 4.92 | 9.76 | 6.89 |
| Dec 2010 | 6.52 | 7.04 | 10.83 | 6.93 | 7.06 | 5.13 | 4.44 | 10.24 | 6.59 |
| Jan 2011 | 5.05 | 4.79 | 9.82 | 5.47 | 4.71 | 5.46 | 2.70 | 11.71 | 5.09 |
| Feb 2011 | 5.19 | 4.79 | 10.73 | 6.20 | 6.47 | 6.62 | 3.65 | 11.71 | 5.39 |
| Mar 2011 | 6.16 | 5.92 | 11.56 | 8.03 | 6.76 | 6.95 | 3.97 | 12.20 | 6.29 |
| Apr 2011 | 7.35 | 7.04 | 12.94 | 9.85 | 7.06 | 8.11 | 4.60 | 11.71 | 7.19 |
| May 2011 | 8.13 | 7.89 | 12.94 | 11.31 | 7.35 | 9.44 | 4.29 | 12.20 | 7.78 |
| Jun 2011 | 8.73 | 8.17 | 13.03 | 11.68 | 7.65 | 9.44 | 3.81 | 13.17 | 8.38 |
| Jul 2011 | 9.51 | 8.45 | 12.29 | 12.41 | 8.24 | 9.11 | 3.97 | 13.66 | 8.98 |
| Aug 2011 | 10.52 | 8.45 | 12.11 | 13.14 | 8.53 | 10.26 | 4.44 | 14.15 | 9.88 |
| Sep 2011 | 11.21 | 10.42 | 13.58 | 14.60 | 9.41 | 10.93 | 4.92 | 15.12 | 9.58 |
| Oct 2011 | 10.56 | 10.70 | 13.49 | 14.96 | 10.59 | 10.93 | 4.92 | 15.61 | 9.28 |
| Nov 2011 | 11.30 | 11.27 | 13.39 | 15.69 | 11.18 | 11.59 | 5.71 | 17.07 | 9.58 |
| Dec 2011 | 11.76 | 12.11 | 13.85 | 16.42 | 11.76 | 11.26 | 5.87 | 18.05 | 9.58 |
| Jan 2012 | 10.20 | 10.99 | 11.65 | 15.69 | 10.00 | 10.60 | 4.76 | 14.15 | 8.08 |
| Feb 2012 | 10.84 | 12.39 | 12.66 | 16.06 | 10.59 | 12.42 | 5.40 | 15.61 | 8.68 |
| Mar 2012 | 11.21 | 13.52 | 14.40 | 17.15 | 12.06 | 13.74 | 5.87 | 16.59 | 9.88 |
| Apr 2012 | 11.44 | 14.08 | 15.50 | 17.88 | 11.76 | 13.91 | 6.51 | 17.56 | 9.28 |
| May 2012 | 11.99 | 14.93 | 17.43 | 19.34 | 12.94 | 15.89 | 6.51 | 19.51 | 10.18 |
| Jun 2012 | 12.40 | 14.93 | 18.72 | 20.80 | 13.82 | 16.23 | 6.19 | 20.49 | 10.78 |
| Jul 2012 | 11.58 | 15.21 | 18.35 | 20.80 | 13.24 | 16.56 | 4.29 | 19.02 | 11.68 |
| Aug 2012 | 12.40 | 14.93 | 19.27 | 21.53 | 14.71 | 18.38 | 4.76 | 19.02 | 12.57 |
| Sep 2012 | 12.17 | 15.77 | 21.01 | 22.99 | 16.76 | 19.37 | 4.92 | 18.05 | 12.57 |
| Oct 2012 | 12.22 | 16.34 | 21.65 | 24.09 | 17.35 | 21.69 | 5.56 | 17.07 | 13.77 |
| Nov 2012 | 12.63 | 16.62 | 20.64 | 24.45 | 15.29 | 22.85 | 6.35 | 17.56 | 14.37 |
| Dec 2012 | 12.72 | 18.31 | 23.67 | 25.91 | 18.82 | 24.17 | 6.83 | 16.59 | 15.27 |
| Jan 2013 | 9.92 | 17.46 | 22.94 | 24.82 | 20.29 | 21.36 | 6.83 | 16.10 | 14.67 |
| Feb 2013 | 10.70 | 17.75 | 23.76 | 25.18 | 20.88 | 22.68 | 7.62 | 16.59 | 15.57 |
| Mar 2013 | 10.98 | 18.87 | 25.69 | 27.37 | 23.82 | 25.00 | 8.25 | 17.07 | 16.77 |
| Apr 2013 | 11.44 | 19.15 | 27.61 | 29.20 | 25.00 | 25.17 | 8.41 | 15.61 | 17.37 |
| May 2013 | 12.26 | 20.56 | 29.08 | 31.02 | 26.18 | 25.50 | 9.21 | 15.61 | 18.56 |
| Jun 2013 | 11.90 | 20.85 | 30.18 | 32.12 | 27.06 | 24.34 | 8.57 | 14.63 | 18.86 |
| Jul 2013 | 12.72 | 21.41 | 30.00 | 31.75 | 22.94 | 25.17 | 7.30 | 14.63 | 17.66 |
| Aug 2013 | 13.55 | 21.69 | 30.18 | 32.48 | 24.12 | 25.50 | 8.41 | 15.12 | 17.96 |
| Sep 2013 | 13.18 | 23.66 | 31.74 | 33.94 | 26.47 | 25.17 | 7.62 | 14.63 | 17.96 |
| Oct 2013 | 13.18 | 24.23 | 34.22 | 34.67 | 25.88 | 25.99 | 8.25 | 13.66 | 16.77 |
| Nov 2013 | 13.64 | 26.20 | 35.50 | 36.13 | 28.24 | 26.49 | 9.52 | 13.66 | 16.77 |
| Dec 2013 | 13.50 | 27.04 | 35.69 | 36.86 | 27.35 | 25.83 | 9.37 | 12.68 | 16.17 |
| Jan 2014 | 11.62 | 25.92 | 35.50 | 35.40 | 26.76 | 26.32 | 6.83 | 11.71 | 15.27 |
| Feb 2014 | 11.85 | 24.51 | 35.96 | 36.13 | 26.18 | 26.66 | 7.94 | 10.73 | 16.47 |
| Mar 2014 | 11.99 | 27.61 | 38.62 | 38.69 | 29.41 | 26.66 | 8.73 | 11.71 | 16.77 |
| Apr 2014 | 12.31 | 29.01 | 39.08 | 41.61 | 29.71 | 26.82 | 9.37 | 10.73 | 15.57 |
| May 2014 | 13.32 | 31.27 | 41.19 | 43.80 | 31.47 | 26.66 | 10.00 | 11.71 | 16.17 |
| Jun 2014 | 13.09 | 31.55 | 42.11 | 45.99 | 33.53 | 26.82 | 9.68 | 9.27 | 15.87 |
| Jul 2014 | 13.18 | 31.55 | 41.56 | 44.89 | 32.06 | 27.15 | 8.25 | 9.76 | 15.27 |
| Aug 2014 | 13.96 | 31.83 | 42.48 | 46.35 | 32.94 | 27.81 | 9.68 | 9.76 | 15.27 |
| Sep 2014 | 14.24 | 34.37 | 44.50 | 48.91 | 35.00 | 28.48 | 10.00 | 8.78 | 15.87 |
| Oct 2014 | 14.61 | 35.77 | 46.24 | 51.46 | 36.18 | 30.63 | 10.48 | 9.76 | 16.77 |
| Nov 2014 | 15.02 | 37.75 | 48.26 | 52.92 | 36.76 | 30.96 | 11.43 | 8.78 | 17.66 |
| Dec 2014 | 15.43 | 37.75 | 49.36 | 54.38 | 37.94 | 31.46 | 11.27 | 8.78 | 17.96 |
| Jan 2015 | 13.64 | 36.90 | 48.26 | 50.73 | 34.12 | 29.14 | 10.63 | 8.78 | 15.57 |
| Feb 2015 | 14.61 | 36.90 | 47.98 | 50.36 | 34.12 | 30.13 | 11.27 | 8.29 | 15.57 |
| Mar 2015 | 14.61 | 38.87 | 50.18 | 53.65 | 37.65 | 30.46 | 12.06 | 7.32 | 16.77 |
| Apr 2015 | 15.53 | 41.13 | 50.83 | 56.57 | 36.76 | 31.79 | 12.86 | 6.83 | 15.87 |
| May 2015 | 16.40 | 43.10 | 52.39 | 59.85 | 39.12 | 32.12 | 13.02 | 6.83 | 16.17 |
| Jun 2015 | 16.72 | 43.66 | 53.67 | 62.04 | 40.00 | 32.45 | 11.75 | 5.85 | 16.77 |
| Jul 2015 | 17.55 | 43.94 | 54.40 | 61.68 | 39.12 | 33.44 | 10.16 | 5.37 | 17.37 |
| Aug 2015 | 18.37 | 43.94 | 54.50 | 63.14 | 39.12 | 34.11 | 10.48 | 4.88 | 17.37 |
| Sep 2015 | 18.79 | 45.92 | 56.79 | 66.06 | 41.47 | 34.93 | 11.59 | 2.93 | 17.37 |
| Oct 2015 | 18.47 | 49.86 | 60.46 | 67.88 | 44.12 | 39.07 | 13.17 | 2.93 | 20.06 |
| Nov 2015 | 19.25 | 50.42 | 62.39 | 68.25 | 46.18 | 39.40 | 14.29 | 3.41 | 20.66 |
| Dec 2015 | 19.66 | 52.96 | 62.57 | 68.98 | 43.53 | 40.89 | 14.60 | 3.41 | 21.26 |
| Jan 2016 | 19.38 | 54.08 | 61.28 | 69.71 | 43.24 | 38.74 | 15.87 | 2.44 | 19.76 |
| Feb 2016 | 21.13 | 54.93 | 62.29 | 69.34 | 39.12 | 40.89 | 16.67 | 1.95 | 17.96 |
| Mar 2016 | 19.66 | 56.06 | 65.05 | 70.44 | 40.29 | 44.21 | 18.25 | .98 | 17.96 |
| Note: The states included in the figure are those for which the Current Employment Statistics program has home health care employment data. Source: U.S. Bureau of Labor Statistics, Current Employment Statistics survey. | |||||||||
| Year | Employment | Medicaid expenditures |
|---|---|---|
| 2000 | 5.8 | 10.5 |
| 2001 | 14.2 | 11.9 |
| 2002 | 11.2 | 10.7 |
| 2003 | 14.0 | 8.4 |
| 2004 | 11.1 | 8.1 |
| 2005 | 10.0 | 6.4 |
| 2006 | 7.7 | -.9 |
| 2007 | 9.7 | 6.3 |
| 2008 | 9.4 | 5.7 |
| 2009 | 7.7 | 8.8 |
| 2010 | 4.2 | 6.1 |
| 2011 | 4.6 | 2.3 |
| 2012 | 9.1 | 3.8 |
| 2013 | 6.0 | 5.9 |
| 2014 | 7.7 | 11.0 |
| Note: Medicaid data are shown as annual average percent change. Current Employment Statistics employment data are shown as percent change from December estimate of current year to December estimate of previous year. Source: U.S. Bureau of Labor Statistics and U.S. Department of Health and Human Services. | ||
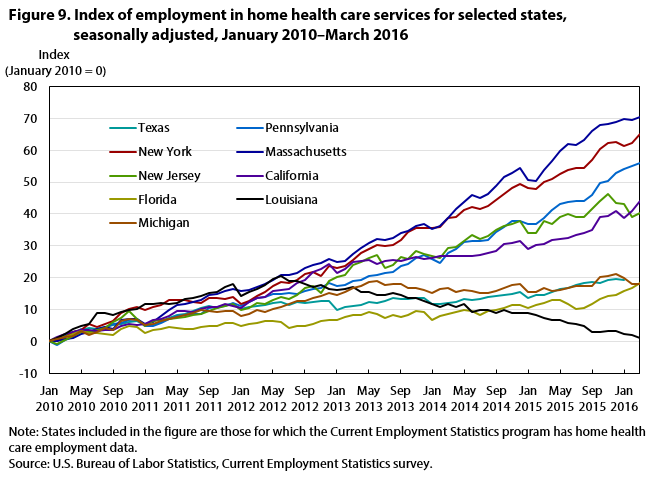
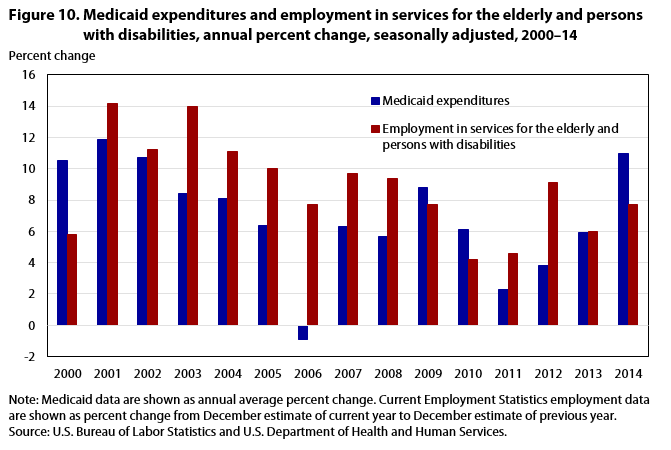
While state plan amendments such as 1915(i) and 1915(k) are generally permanent after implementation, other, similar initiatives are temporary. One such initiative is the Balancing Incentive Program, which increased Medicaid’s Federal Matching Assistance Percentage for states that (1) improved accessibility to community-based care services and (2) successfully increased the portion of their Medicaid long-term care budget spent on community-based care services, to 50 percent by September 2015. From October 2011 to September 2015, the program gave $2.4 billion in enhanced federal payments for community-based care services to participating states.22 States that participated in the initiative for its full duration had higher employment growth in home health care services—the community-based care industry for which the Current Employment Statistics program has the richest state-level data—than states that did not fully participate.23 (See figure 9.) At the national level, increases in Medicaid expenditures correlated positively with job increases in services for the elderly and persons with disabilities.24 (See figure 10.)
| Date | Employment (thousands) |
|---|---|
| Jan 2010 | 1,648.4 |
| Feb 2010 | 1,650.8 |
| Mar 2010 | 1,653.6 |
| Apr 2010 | 1,655.5 |
| May 2010 | 1,655.7 |
| Jun 2010 | 1,655.2 |
| Jul 2010 | 1,658.6 |
| Aug 2010 | 1,659.3 |
| Sep 2010 | 1,659.2 |
| Oct 2010 | 1,660.1 |
| Nov 2010 | 1,667.2 |
| Dec 2010 | 1,668.4 |
| Jan 2011 | 1,668.8 |
| Feb 2011 | 1,667.9 |
| Mar 2011 | 1,668.7 |
| Apr 2011 | 1,669.1 |
| May 2011 | 1,669.5 |
| Jun 2011 | 1,673.1 |
| Jul 2011 | 1,672.2 |
| Aug 2011 | 1,672.9 |
| Sep 2011 | 1,673.6 |
| Oct 2011 | 1,671.5 |
| Nov 2011 | 1,664.5 |
| Dec 2011 | 1,664.3 |
| Jan 2012 | 1,666.7 |
| Feb 2012 | 1,663.6 |
| Mar 2012 | 1,668.3 |
| Apr 2012 | 1,664.3 |
| May 2012 | 1,664.9 |
| Jun 2012 | 1,662.5 |
| Jul 2012 | 1,663.1 |
| Aug 2012 | 1,657.6 |
| Sep 2012 | 1,660.4 |
| Oct 2012 | 1,658.1 |
| Nov 2012 | 1,657.6 |
| Dec 2012 | 1,661.4 |
| Jan 2013 | 1,655.3 |
| Feb 2013 | 1,658.5 |
| Mar 2013 | 1,657.5 |
| Apr 2013 | 1,656.7 |
| May 2013 | 1,654.2 |
| Jun 2013 | 1,653.4 |
| Jul 2013 | 1,649.6 |
| Aug 2013 | 1,657.2 |
| Sep 2013 | 1,649.2 |
| Oct 2013 | 1,651.2 |
| Nov 2013 | 1,649.5 |
| Dec 2013 | 1,648.3 |
| Jan 2014 | 1,648.1 |
| Feb 2014 | 1,650.4 |
| Mar 2014 | 1,649.0 |
| Apr 2014 | 1,651.4 |
| May 2014 | 1,652.0 |
| Jun 2014 | 1,653.2 |
| Jul 2014 | 1,651.3 |
| Aug 2014 | 1,649.7 |
| Sep 2014 | 1,648.7 |
| Oct 2014 | 1,648.4 |
| Nov 2014 | 1,649.0 |
| Dec 2014 | 1,649.3 |
| Jan 2015 | 1,652.8 |
| Feb 2015 | 1,650.8 |
| Mar 2015 | 1,644.6 |
| Apr 2015 | 1,647.9 |
| May 2015 | 1,648.1 |
| Jun 2015 | 1,648.9 |
| Jul 2015 | 1,652.9 |
| Aug 2015 | 1,655.1 |
| Sep 2015 | 1,657.1 |
| Oct 2015 | 1,657.1 |
| Nov 2015 | 1,659.2 |
| Dec 2015 | 1,659.7 |
| Jan 2016 | 1,655.3 |
| Source: U.S. Bureau of Labor Statistics, Current Employment Statistics survey. | |
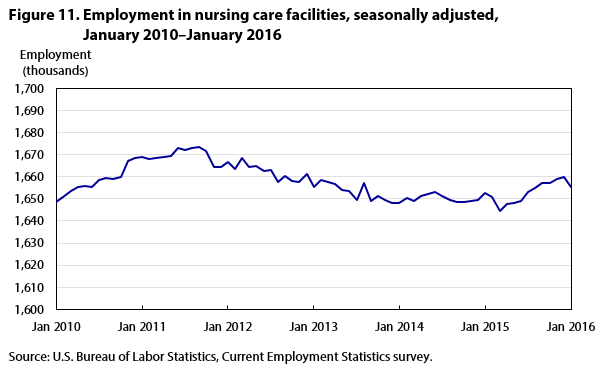
While employment growth in community-based care industries has strengthened, that in nursing care facilities has weakened. At the end of 2015, employment in nursing care facilities was still 14,000 below its peak in September 2011. (See figure 11.) One reason for this slower growth is Medicare market-basket reductions for inpatient services.25 These reductions, which began in 2010, lowered the Medicare payments made for inpatient services, the primary services provided by nursing care facilities. In addition, the expansion of service coverage in community-based care industries may have caused a higher proportion of aging adults to receive services in these industries instead of in nursing care facilities.
Employment growth in the health care and social assistance sector continues to be strong. Much of this growth has been concentrated in three community-based care industries, namely, home health care services, services for the elderly and persons with disabilities, and community care facilities for the elderly. As these component industries have added jobs at a rapid pace, they have also driven the expansion of a few low-wage occupations that typically do not require an educational credential for entry. These employment and occupational changes reflect long-term trends relevant to the present and future needs of the aging baby-boom generation.
The job growth in community-based care industries, which are labor intensive, is correlated with an increased demand for their services. This demand has been driven by a combination of economic, demographic, and legislative factors. Community-based care services are less expensive than other types of elder care, and this difference in cost has made them a more attractive option for the growing population of Americans ages 65 and older. In addition, legislative changes introduced since the implementation of the ACA have increased funding for community-based care and improved its accessibility.
Kara Sullivan, "Workforce growth in community-based care: meeting the needs of an aging population," Monthly Labor Review, U.S. Bureau of Labor Statistics, December 2016, https://doi.org/10.21916/mlr.2016.53
1 Catherine A. Wood, “Employment in health care: a crutch for the ailing economy during the 2007–09 recession,” Monthly Labor Review, April 2011, https://www.bls.gov/opub/mlr/2011/04/art2full.pdf.
2 Unless otherwise noted, employment data in this article are from the Current Employment Statistics (CES) survey.
3 Understanding Medicaid home and community services: a primer (U.S. Department of Health and Human Services, October 2010), https://aspe.hhs.gov/sites/default/files/pdf/73101/primer.pdf.
4 “Community care facilities for the elderly” is a title used by CES for NAICS 6233 (continuing care retirement communities and assisted living facilities for the elderly).
5 This job gain coincided with a reconstruction in the industry’s data series. The Quarterly Census of Employment and Wages (QCEW) program determined that employment from a number of state programs that provide funding for the industry was incorrectly coded as being in private households. With the first quarter of 2013, QCEW began coding this employment under services for the elderly and persons with disabilities. Six states—California, Massachusetts, Missouri, Nebraska, Texas, and Washington—had employment reconstructions in this industry. For more information on these reconstructions, see Wade Petty and Patrick Hu, “CES—national benchmark article: BLS establishment survey national estimates revised to incorporate March 2013 benchmarks” (U.S. Bureau of Labor Statistics, 2013), https://www.bls.gov/ces/cesbmart13.pdf.
6 Lam Thuy Vo and Josh Zumbrun, “Just how good (or bad) are all the jobs added to the economy since the recession?” The Wall Street Journal, May 11, 2016.
7 “May 2015 occupation profiles,” Occupational Employment Statistics (U.S. Bureau of Labor Statistics), https://www.bls.gov/oes/current/oes_stru.htm.
8 “May 2015 national industry-specific occupational employment and wage estimates,” Occupational Employment Statistics (U.S. Bureau of Labor Statistics), https://www.bls.gov/oes/current/oessrci.htm.
9 Andrew Hogan and Brian Roberts, “Occupational employment projections to 2024,” Monthly Labor Review, December 2015, https://www.bls.gov/opub/mlr/2015/article/occupational-employment-projections-to-2024.htm.
10 “Intercensal estimates” (U.S. Census Bureau), https://www.census.gov/popest/data/intercensal/index.html; and “Current estimates data” (U.S. Census Bureau), https://www.census.gov/popest/data/index.html.
11 A profile of older Americans: 2014 (U.S. Department of Health and Human Services), http://www.aoa.acl.gov/aging_statistics/Profile/2014/docs/2014-Profile.pdf.
12 Ibid.
13 “Table 1300. Age of reference person: annual expenditure means, shares, standard errors, and coefficients of variation, Consumer Expenditure Survey, 2014” (U.S. Bureau of Labor Statistics, September 2015), https://www.bls.gov/cex/2014/combined/age.pdf.
14 “Genworth 2015 Cost of Care Survey” (Genworth Financial, Inc., April 1, 2015), https://www.genworth.com/dam/Americas/US/PDFs/Consumer/corporate/130568_040115_gnw.pdf.
15 Data are for the Consumer Price Index for All Urban Consumers and are not seasonally adjusted. See “CPI databases,” Consumer Price Index (U.S. Bureau of Labor Statistics), https://www.bls.gov/cpi/data.htm.
16 Duggan v. Bowen, U.S. District Court for the District of Columbia, no. 87-0383, August 1, 1988.
17 Nelda McCall, “Long term care: definition, demand, cost, and financing,” in Nelda McCall, ed., Who will pay for long term care? Insights from the Partnership programs (Chicago, IL: Health Administration Press, 2001), p. 19.
18 “Fact sheet: summary of key provisions of the final rule for 1915(i) Home and Community-Based Services (HCBS) state plan option” (U.S. Department of Health and Human Services, January 10, 2014).
19 “Improving access to home and community-based services” (U.S. Department of Health and Human Services, August 6, 2010), https://openminds.com/wp-content/uploads/indres/080610dscmshcbs.pdf.
20 “Medicaid program; State Plan Home and Community-Based Services, 5-year period for waivers, provider payment reassignment, and home and community-based setting requirements for Community First Choice and Home and Community-Based Services (HCBS) waivers; final rule,” Federal Register, vol. 79, no. 11, January 16, 2014, pp. 2947–3039, https://federalregister.gov/a/2014-00487.
21 “Medicaid program; Community First Choice Option; final rule,” Federal Register, vol. 77, no. 88, May 7, 2012, pp. 26827–26903, https://www.federalregister.gov/documents/2012/05/07/2012-10294/medicaid-program-community-first-choice-option.
22 See “Balancing Incentive Program” (U.S. Department of Health and Human Services), https://www.medicaid.gov/Medicaid-CHIP-Program-Information/By-Topics/Long-Term-Services-and-Supports/Balancing/Balancing-Incentive-Program.html. The following states continued participating in the program after the September 2015 deadline: Connecticut, Georgia, Illinois, Maine, Maryland, Massachusetts, Mississippi, Nevada, New Hampshire, New Jersey, New York, Pennsylvania, and Texas.
23 As shown in figure 9, California still has high employment growth in home health care services, despite not participating in the Balancing Incentive Program. This could be due to demographic and other factors specific to the state’s healthcare system.
24 “Table 3. National health expenditures; levels and annual percent change, by source of funds: selected calendar years 1960–2014” (U.S. Department of Health and Human Services), https://www.cms.gov/research-statistics-data-and-systems/statistics-trends-and-reports/nationalhealthexpenddata/nhe-fact-sheet.html.
25 A “market basket” is an index measuring changes in the cost of goods and services—in this case, purchased by inpatient facilities. See “Market basket definitions and general information” (U.S. Department of Health and Human Services), https://www.cms.gov/research-statistics-data-and-systems/statistics-trends-and-reports/medicareprogramratesstats/downloads/info.pdf.