An official website of the United States government
 United States Department of Labor
United States Department of Labor

Crossref 0
The relationship between physical work hazards and employee withdrawal: The moderating role of safety compliance, Stress and Health, 2019.
Occupational Injuries and Their Determinants Among Healthcare Workers in Western Countries: A Scoping Review, La Medicina del Lavoro, 2025.
An Investigation of Healthcare Worker Perception of Their Workplace Safety and Incidence of Injury, Workplace Health & Safety, 2020.
Emory Healthcare’s Safe Patient Handling Program, Advances in Human Factors and Ergonomics in Healthcare and Medical Devices, 2019.
EXPO-S.T.O.P. 2016 and 2017 blood exposure surveys: An alarming rise, American Journal of Infection Control, 2019.
Occupational injuries and illnesses among registered nurses, Monthly Labor Review, 2018.
Adoption of a Data‐Driven Bayesian Belief Network Investigating Organizational Factors that Influence Patient Safety, Risk Analysis, 2022.
PAs' experience with violence and bias, JAAPA, 2025.
Corporate Cruelty: Holding Factory Farms Accountable for Animal Cruelty Crimes to Encourage Systemic Reform, SSRN Electronic Journal , 2019.
A tailored, interdisciplinary, multicomponent approach to decreasing workers’ compensation claims and costs in a hospital system: A retrospective study, Journal of Healthcare Risk Management, 2023.
The Comorbidity of Musculoskeletal Disorders and Depression: Associations with Working Conditions Among Hospital Nurses, Workplace Health & Safety, 2020.
Protocol of a scoping review assessing injury rates and their determinants among healthcare workers in western countries, BMJ Open, 2019.
Job and family demands and burnout among healthcare workers: The moderating role of workplace flexibility, SSM - Population Health, 2021.
Using Behavioral Theory to Enhance Occupational Safety and Health: Applications to Health Care Workers, American Journal of Lifestyle Medicine, 2021.
Predictive Risk Modelling and Occupational Hazard Mapping in the United States Healthcare Sector: A Data-Driven Safety Surveillance Study, European Journal of Medical and Health Research, 2023.
System Approach for Characterizing and Evaluating Factors for Occupational Health Impacts Due to Nonfatal Injuries and Illnesses for the Use in Life Cycle Assessment, Environmental Science & Technology, 2023.
Private industry hospital workers exhibit a higher incidence of injury and illness—6.0 cases per 100 full-time workers—than employees working in other industries traditionally considered dangerous, such as manufacturing and construction. Hospital workers routinely face hazards related to lifting, moving, or otherwise physically interacting with patients. Workplace injuries and illnesses among hospital workers reflect common risks of hospital jobs and differ by type of hospital.
In terms of employment, the health care and social assistance sector is one of the largest service-providing sectors in the U.S. economy.1 It is projected to be the fastest growing sector through 2024, with healthcare occupations expected to add more jobs than any other occupational group.2 In addition to playing a significant role in national employment, the health care sector plays a vital role in promoting public health. Its services include treating illnesses and injuries, maintaining wellness, and managing disease.3
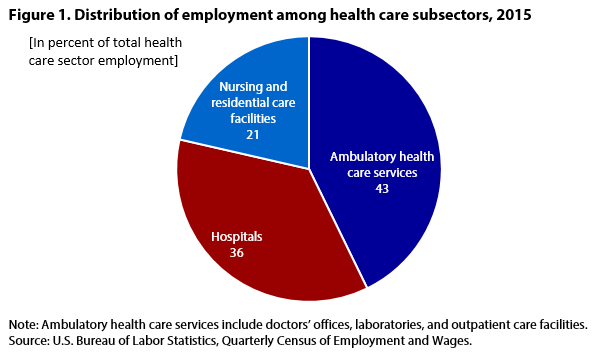
| Health care subsector | Employment (percent of total health care sector employment) |
|---|---|
| Ambulatory health care services | 42.8 |
| Hospitals | 35.8 |
| Nursing and residential care facilities | 21.4 |
| Note: Ambulatory health care services include doctors’ offices, laboratories, and outpatient care facilities. Source: U.S. Bureau of Labor Statistics, Quarterly Census of Employment and Wages. | |
Numerous industries compose the health care sector, including offices of physicians, outpatient care centers, home health care services, hospitals, and nursing and residential care facilities. Of the three major health care industry categories—ambulatory health care services, hospitals, and nursing and residential care facilities—hospitals accounted for about 36 percent of total healthcare jobs in 2015.4 (See figure 1.) Hospitals employ workers in diverse occupations, including nurses, cooks, and maintenance workers.5
Because of the physical nature of many hospital jobs, private industry hospital employees face a higher incidence of injury and illness—6.0 cases per 100 full-time workers—than employees working in other industries traditionally considered dangerous, such as manufacturing and construction.6 In addition, the injuries of hospital workers tend to carry substantial financial costs. An Occupational Safety and Health Administration (OSHA) report using data on worker compensation claims from the Aon barometer survey estimated that the average loss per claim settled for hospital workers’ injuries in 2011 was $15,860.7 Other studies cited in the report also point to high financial and societal costs associated with replacing nurses who leave the profession because of workplace injuries or illnesses.
This article analyzes injury and illness counts and incidence rates among workers employed in different types of hospitals.8 It also sheds light on the kinds of workplace injuries and illnesses incurred by hospital employees.
All nonfatal occupational injury and illness data presented in this article come from the Survey of Occupational Injuries and Illnesses (SOII), which is conducted by the U.S. Bureau of Labor Statistics (BLS).9 Data from the BLS Census of Fatal Occupational Injuries (CFOI), which provides a complete count of fatal occupational injuries, are also referenced in the analysis.10 Because hospitals in the SOII are commonly grouped by “ownership” (private industry, state government, and local government), the article compares the injury and illness experiences of workers employed in hospitals of different ownerships. Analysis is also provided for hospitals classified under different North American Industry Classification System (NAICS) categories within each ownership.
The SOII is a federal–state cooperative program administered by BLS in cooperation with state agencies. Employers report, on an annual basis, injury and illness data for approximately 230,000 establishments in private industry and state and local government.11 Definitions of recordable injury and illness cases for the SOII conform to guidelines set by OSHA.12 The SOII also collects details of case circumstances and worker demographics for cases that result in days away from work and, for selected industries, for cases involving days of job transfer or restriction.13
The Occupational Injury and Illness Classification System (OIICS), developed by BLS, provides a standardized coding system for characterizing the case circumstances of both nonfatal work-related injuries and illnesses from the SOII and fatal workplace injuries from the CFOI.14 The OIICS uses the following characteristics to describe an occupational injury or illness case: the “nature,” or type, of injury or illness; “event or exposure”; “part of body affected”; and “source or secondary source,” such as machinery, equipment, or other factors that precipitated the event or exposure.
Data used to measure the number of hospital establishments are from the BLS Quarterly Census of Employment and Wages (QCEW) program, which publishes a quarterly count of employment and wages reported by employers.15 The QCEW covers 98 percent of U.S. jobs, providing data, by industry, at the county, Metropolitan Statistical Area, and state and national levels.16
Incidence rates of nonfatal workplace injuries and illnesses vary significantly by type of hospital. Hospitals are classified according to the NAICS and fall under the NAICS 622 subsector, which is further broken down into general medical and surgical hospitals (NAICS 6221), psychiatric and substance abuse hospitals (NAICS 6222), and specialty (except psychiatric and substance abuse) hospitals (NAICS 6223).17 All three types of hospitals provide diagnostic and medical treatment, are equipped for inpatient care (maintaining beds and providing food services to patients), and offer additional services (such as outpatient services, clinical laboratory services, and diagnostic X-ray services). All hospital establishments maintain a staff of physicians and other medical care providers.
The different types of hospitals vary by the services they offer. General medical and surgical hospitals offer the most diverse operating room services for a variety of procedures, while psychiatric and substance abuse hospitals offer mental health services in areas such as psychiatry, psychology, and social work. Specialty hospitals are distinctive in that they typically provide diagnostic and medical treatment to patients with a specific type of disease or medical condition (excluding psychiatric and substance abuse conditions). They also may provide long-term care for the chronically ill and rehabilitation, restorative, and adjustive services to physically challenged people or people with disabilities. Specific services offered in these areas include physical therapy, educational and vocational services, and psychological and social work services.
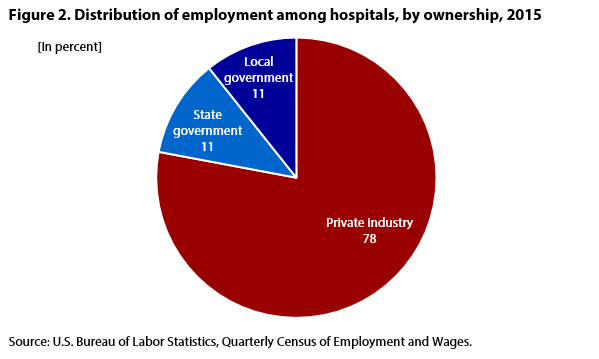
| Ownership | Employment (percent) |
|---|---|
| Private industry | 78.0 |
| State government | 11.3 |
| Local government | 10.7 |
| Source: U.S. Bureau of Labor Statistics, Quarterly Census of Employment and Wages. | |
Hospitals also can be broken down by the three ownership types measured by the SOII: private industry, state government, and local government. (Federal hospitals are not within the scope of the SOII.) Figure 2 shows the percent distribution of employment among hospitals of different ownership types. Nonprofit hospitals account for more than half of private industry hospitals.18
In 2015, hospitals in two of the three ownership categories reported worker injury and illness incidence rates above the total industry average for their respective ownerships. (See figure 3.) The incidence rate for workers in state government hospitals was 8.1 cases per 100 full-time workers, significantly higher than the incidence rate among workers in all state government establishments (3.7 cases per 100 full-time workers). Private hospitals also had an incidence rate (6.0 cases per 100 full-time workers) that was significantly higher than the average rate for all private industry establishments (3.0 cases per 100 full-time workers). Local government hospitals exhibited a rate of injury and illness that was lower (5.2 cases per 100 full-time workers) than that for private and state-run hospitals and also lower than the average rate for all local government establishments (5.6 cases per 100 full-time workers).
| Ownership | Rate for ownership | Rate for hospitals in ownership |
|---|---|---|
| Private industry | 3.0 | 6.0 |
| State government | 3.7 | 8.1 |
| Local government | 5.6 | 5.2 |
| Note: Incidence rates represent the number of injuries and illnesses per 100 full-time workers. Source: U.S. Bureau of Labor Statistics, Survey of Occupational Injuries and Illnesses. | ||
Although the SOII does not provide injury and illness rates for different NAICS categories of state government and local government hospitals, the prevalence of certain types of hospitals in each ownership category may contribute to the rate differentials observed in figure 3. Staff of private and local government medical and surgical hospitals often face hazardous physical tasks involving lifting and moving patients. Similar tasks may be common in hospitals across all ownerships; however, psychiatric and substance abuse hospitals, which are more prevalent among state-run facilities, lend themselves to higher employee injury and illness rates, because psychiatric technicians and aides care for patients whose illnesses may lead to disoriented, uncooperative, or violent behaviors.19
In 2015, about 72 percent of private industry hospitals were medical and surgical hospitals.20 Of the remaining private hospitals, 17 percent were specialty hospitals and 11 percent were psychiatric and substance abuse hospitals.21 Local government hospitals had an even higher share of medical and surgical hospitals, 98 percent, with the remaining 2 percent divided between psychiatric and specialty hospitals.22 The composition of state government hospitals contrasts sharply with that of private and local government hospitals. The vast majority of state-run hospitals, 78 percent, were psychiatric and substance abuse hospitals,23 14 percent were specialty hospitals, and 8 percent were general medical and surgical hospitals.24 (See figure 4.)
| NAICS category | Private hospitals | State government hospitals | Local government hospitals |
|---|---|---|---|
| Medical and surgical | 71.9 | 7.9 | 98.4 |
| Psychiatric and substance abuse | 10.7 | 77.8 | 1.2 |
| Specialty | 17.4 | 14.3 | 0.5 |
| Note: Percentages may not add to 100 because of rounding. North American Industry Classification System (NAICS) 622 (hospitals) is broken down into NAICS 6221 (general medical and surgical hospitals), NAICS 6222 (psychiatric and substance abuse hospitals), and NAICS 6223 (specialty [except psychiatric and substance abuse] hospitals). Source: U.S. Bureau of Labor Statistics, Quarterly Census of Employment and Wages. | |||
Examining data on case circumstances and worker characteristics for SOII cases resulting in days away from work provides a more detailed insight into the injuries and illnesses suffered by hospital workers. The OIICS manual identifies case circumstances in terms of an incident’s “event or exposure,” defined as “the manner in which the injury or illness was produced or inflicted by the source of injury or illness.”25 In that definition, the term “source” refers to “the objects, substances, equipment, and other factors that were responsible for the injury or illness.”26
In hospitals, the most prevalent event leading to nonfatal injuries and illnesses varies by hospital ownership. (See figure 5.) For private industry and local government hospitals, which are predominantly medical and surgical hospitals, the most common event leading to injuries in 2015 was overexertion and bodily reaction, which includes injuries from lifting or moving patients. This event accounted for 45 percent of cases (24,040) in private hospitals and 44 percent of cases (3,090) in local government hospitals. The second most common event leading to workplace injuries and illnesses in private industry and local government hospitals was falls, slips, and trips. This event represented 25 percent of cases (13,230) in private hospitals and 24 percent of cases (1,690) in local government hospitals.
| Event or exposure | Private hospitals | State government hospitals | Local government hospitals |
|---|---|---|---|
| Overexertion and bodily reaction | 45.1 | 26.1 | 43.9 |
| Falls, slips, and trips | 24.8 | 14.9 | 24.0 |
| Violence and other injuries by persons or animals | 11.0 | 45.9 | 14.8 |
| Contact with object or equipment | 13.7 | 10.0 | 10.9 |
| Exposure to harmful substances or environments | 4.2 | 2.2 | 4.8 |
| Transportation incidents | 1.1 | 0.8 | 1.3 |
| All other | 0.1 | 0.2 | 0.3 |
| Note: Percentages may not add to 100 because of rounding. Source: U.S. Bureau of Labor Statistics, Survey of Occupational Injuries and Illnesses. | |||
Among state-run hospitals, which are predominantly psychiatric and substance abuse hospitals, the most common event leading to injuries in 2015 was violence and other injuries by persons or animals (4,590 cases). This event includes all intentional injuries; injuries involving weapons, regardless whether intentional or unintentional; and injuries involving direct physical contact with persons, animals, or insects, regardless of intent. Over half of these injuries (3,050 cases) were subclassified as “intentional injuries by other person.” The second most common event leading to injuries in state government hospitals in 2015 was overexertion and bodily reaction (2,610 cases), which was the most common event for hospitals of other ownerships. The distinctive event distribution of state-run hospitals may be due to the high concentration of psychiatric and substance abuse establishments in this ownership group. As noted previously, workers in psychiatric hospitals are more likely to suffer injuries caused by the violence of others.
The most common source of nonfatal injury or illness resulting in days away from work among all three hospital ownerships in 2015 was a “person other than injured or ill worker.” (See table 1.) This source accounted for 57 percent, 35 percent, and 34 percent of cases in state government, local government, and private industry hospitals, respectively. In the majority of cases, the source was further identified as “healthcare patients.” Thus, many injuries were sustained during physical interactions such as lifting and moving patients.
| Source of injury | Private hospitals | State government hospitals | Local government hospitals |
|---|---|---|---|
| Person other than injured or ill worker | 33.9 | 57.1 | 34.8 |
| Floors, walkways, and ground surfaces | 19.2 | 12.4 | 18.6 |
| Person injured or ill worker | 12.5 | 7.9 | 14.1 |
| All other | 10.8 | 7.2 | 10.9 |
| Furniture fixtures | 6.8 | 3.6 | 5.5 |
| Containers | 6.4 | 3.3 | 6.0 |
| Vehicles | 3.9 | 4.1 | 3.3 |
| Machinery | 2.4 | 1.2 | 1.6 |
| Chemicals and chemical products | 1.7 | 0.6 | 2.7 |
| Handtools | 1.1 | 0.9 | 0.9 |
| Parts and materials | 0.9 | 1.2 | 1.3 |
| Ladders | 0.4 | 0.4 | 0.7 |
| Note: Percentages may not add to 100 because of rounding. Source: U.S. Bureau of Labor Statistics, Survey of Occupational Injuries and Illnesses. | |||
In 2015, sprains, strains, and tears represented the most common “nature” of nonfatal injury or illness among all types of private industry, state government, and local government hospitals. The nature of a work-related injury or illness identifies the principal physical characteristic(s) or symptom(s) of that injury or illness. Many of the sprains, strains, and tears sustained by hospital workers in 2015 were serious, most often resulting in 31 or more days away from work. (See figure 6.)
| Number of days away from work | Private hospitals | State government hospitals | Local government hospitals |
|---|---|---|---|
| 1 day | 13.4 | 13.8 | 13.1 |
| 2 days | 10.7 | 8.5 | 11.5 |
| 3–5 days | 19.4 | 15.3 | 21.2 |
| 6–10 days | 13.9 | 13.3 | 11.8 |
| 11–20 days | 12.1 | 12.0 | 10.5 |
| 21–30 days | 6.5 | 6.3 | 5.8 |
| 31 or more days | 23.9 | 30.9 | 26.1 |
| Note: Percentages may not add to 100 because of rounding. Source: U.S. Bureau of Labor Statistics, Survey of Occupational Injuries and Illnesses. | |||
Injury and illness similarities among hospitals of different ownerships were also observed with respect to the part of body affected, defined by the OIICS as “the part of the body directly affected by the previously identified nature of injury or illness.”27 (See table 2.) These similarities were particularly pronounced between local government and private industry hospitals. In 2015, injuries to the trunk were common across all hospital ownerships, with back injuries representing the majority of cases. Many injuries also occurred to upper extremities, such as hands and shoulders, and lower extremities, such as legs, feet, and ankles.
| Part of body | Private hospitals | State government hospitals | Local government hospitals |
|---|---|---|---|
| Trunk | 30.3 | 20.2 | 28.6 |
| Upper extremities | 27.5 | 22.4 | 24.1 |
| Lower extremities | 19.2 | 16.8 | 18.0 |
| Multiple | 12.7 | 23.8 | 16.1 |
| Head | 6.0 | 12.8 | 8.1 |
| Neck | 1.9 | 1.7 | 1.7 |
| Body systems | 1.9 | 1.5 | 3.0 |
| All other | 0.4 | 0.9 | 0.4 |
| Note: Percentages may not add to 100 because of rounding. Source: U.S. Bureau of Labor Statistics, Survey of Occupational Injuries and Illnesses. | |||
Compared with nonfatal injuries, fatal workplace injuries are relatively rare, because the types of injuries and illnesses commonly occurring in hospitals (see earlier discussion) generally do not result in fatal outcomes. In 2015, there were 24 fatal work-related injuries in hospitals, 21 of which occurred in private hospitals and 3 in government hospitals.28 Only five fatal cases resulted from violence and other injuries by persons or animals, an event responsible for a large number of nonfatal cases.29 Other events or exposures leading to fatal workplace injuries in 2015 included transportation incidents (nine injuries); falls, slips, and trips (seven injuries); and exposure to harmful substances or environments (three injuries).30
This article highlights the high prevalence of injuries and illnesses among hospital workers. It also examines how the characteristics and circumstances of those injuries and illnesses vary across hospitals of different service and ownership types. The analysis provides illustrative examples of the data available for studying workplace safety in hospitals.
Researching hospital injury and illness incidence rates presents various challenges. Currently, the SOII does not provide aggregate measures of injuries and illnesses for all three hospital ownerships. In addition, the services offered by different types of hospitals may be “intermixed.” For example, psychiatric services might sometimes be included as a subunit in a general medical and surgical hospital; in such cases, injury and illness statistics specific to that subunit would not be differentiated from those for the entire establishment. Lastly, injury and illness rates for contracted hospital workers (e.g., visiting doctors or emergency medical technicians) may not be included in hospital incident reports, because such workers generally report their injuries to their employer (a contractor) rather than the hospital in which the injury was incurred.
Michelle A. Dressner, "Hospital workers: an assessment of occupational injuries and illnesses," Monthly Labor Review, U.S. Bureau of Labor Statistics, June 2017, https://doi.org/10.21916/mlr.2017.17
1 Richard Henderson, “Industry employment and output projections to 2024,” Monthly Labor Review, December 2015, https://www.bls.gov/opub/mlr/2015/article/industry-employment-and-output-projections-to-2024.htm.
2 Ibid. For additional information on healthcare occupations, see “Healthcare occupations,” Occupational outlook handbook (U.S. Bureau of Labor Statistics, December 17, 2015), https://www.bls.gov/ooh/healthcare/home.htm. The handbook is revised every 2 years by economists in the Employment Projections program of the U.S. Bureau of Labor Statistics (BLS).
3 Elka Torpey, “Healthcare: millions of jobs now and in the future,” Occupational Outlook Quarterly (U.S. Bureau of Labor Statistics, Spring 2014), https://www.bls.gov/careeroutlook/2014/spring/art03.pdf.
4 These estimates were obtained by first combining employment for 2012 North American Industry Classification System (NAICS) sectors 621 (ambulatory health care services), 622 (hospitals), and 633 (nursing and residential care facilities) and then calculating the percentage of workers in NAICS 622. Employment data are from the BLS Quarterly Census of Employment and Wages (QCEW) and cover establishments with state government, local government, and private industry ownership. NAICS 621 includes doctors’ offices, laboratories, and outpatient care centers.
5 “OES data,” Occupational Employment Statistics (U.S. Bureau of Labor Statistics, May 2015), https://www.bls.gov/oes/tables.htm.
6 Incidence rates are compared across private hospitals, private construction industries, and private manufacturing industries.
7 See Caring for our caregivers: facts about hospital worker safety (U.S. Department of Labor, Occupational Safety and Health Administration, September 2013), section 4, “Why it matters,” https://www.osha.gov/dsg/hospitals/documents/1.2_Factbook_508.pdf. See also Martha B. Posey, Gregory Larcher, and Virginia Newton, “2012 health care workers compensation barometer: actuarial analysis” (Aon Risk Solutions, September 2012), http://www.aon.com/attachments/risk-services/2012-HC-WorkersComp_Barometer_Report_Abridged.pdf.
8 The incidence rates represent the number of injuries and illnesses per 100 full-time workers and were calculated as follows: (N/EH) × 200,000, where N = number of injuries, EH = total hours worked by all employees during the calendar year, 200,000 = base for 100 equivalent full-time workers (working 40 hours per week, 50 weeks per year).
9 “Nonfatal occupational injuries and illnesses by industry,” Injuries, Illnesses, and Fatalities (U.S. Bureau of Labor Statistics), https://www.bls.gov/iif/oshsum1.htm.
10 “Census of Fatal Occupational Injuries (CFOI),” Injuries, Illnesses, and Fatalities (U.S. Bureau of Labor Statistics), https://www.bls.gov/iif/oshfat1.htm. The scope of the CFOI differs from that of the SOII. For further information on methodology and scope, see Handbook of methods (U.S. Bureau of Labor Statistics), chapter 9, “Occupational safety and health statistics,” https://www.bls.gov/opub/hom/pdf/homch9.pdf.
11 “Nonfatal occupational injuries and illnesses by industry,” Injuries, Illnesses, and Fatalities (U.S. Bureau of Labor Statistics), https://www.bls.gov/iif/oshsum1.htm.
12 “OSHA injury and illness recordkeeping and reporting requirements” (U.S. Department of Labor, Occupational Safety and Health Administration), https://www.osha.gov/recordkeeping/index.html. OSHA differentiates between (1) cases involving days away from work or days of restricted work activity (or both) beyond the day of injury or onset of illness and (2) other recordable cases that do not result in lost work time.
13 “Nonfatal occupational injuries and illnesses by case circumstances and worker characteristics,” Injuries, Illnesses, and Fatalities (U.S. Bureau of Labor Statistics), https://www.bls.gov/iif/oshcase1.htm.
14 “Occupational Injury and Illness Classification System, version 2.01,” Injuries, Illnesses, and Fatalities (U.S. Bureau of Labor Statistics), https://www.bls.gov/iif/oshoiics.htm.
15 Quarterly Census of Employment and Wages (U.S. Bureau of Labor Statistics), https://www.bls.gov/cew/.
16 Ibid.
17 For further information on the NAICS, see “Introduction to NAICS,” North American Industry Classification System (U.S. Census Bureau), https://www.census.gov/eos/www/naics/.
18 “Fast facts on U.S. hospitals” (Chicago, IL: American Hospital Association, 2017), http://www.aha.org/research/rc/stat-studies/fast-facts.shtml. Data are from the 2015 AHA Annual Survey of Hospitals.
19 For more information, see “Psychiatric technicians and aides,” Occupational outlook handbook (U.S. Bureau of Labor Statistics, December 17, 2015), https://www.bls.gov/ooh/healthcare/psychiatric-technicians-and-aides.htm.
20 Annual 2015 QCEW data for NAICS 622 (hospitals), NAICS 6221 (general medical and surgical hospitals), NAICS 6222 (psychiatric and substance abuse hospitals), and NAICS 6223 (specialty [except psychiatric and substance abuse] hospitals).
21 Ibid.
22 Ibid.
23 Ibid.
24 Ibid.
25 Occupational injury and illness classification manual (U.S. Bureau of Labor Statistics, January 2012), p. 274, https://www.bls.gov/iif/oiics_manual_2010.pdf.
26 Ibid., p. 106.
27 Ibid., p. 82.
28 Data are from “2015 Census of Fatal Occupational Injuries,” Injuries, Illnesses, and Fatalities (U.S. Bureau of Labor Statistics), https://www.bls.gov/iif/oshfat1.htm. The CFOI combines different types of government ownerships under the single category “government.”
29 Ibid.
30 Ibid.